Results from the Migraine in Aotearoa New Zealand Survey 2022
When we go to the doctor to get something that might help reduce the number of migraine attacks we’re getting, we usually expect a prescription for a pill. Nowadays, we might be wanting to try the new calcitonin gene-related peptide (CGRP) medications, like Emgality, given as an injection once every four weeks.
But there are other injections used to prevent migraine that have been around for many years before Emgality was invented.
Occipital nerve blocks
An occipital nerve block involves injecting local anaesthetic into the nerves at the back of the head, the occipital nerves. The aim of this treatment is to block the nerves from transmitting pain signals, hence these injections are called occipital nerve blocks. They’ve been found to reduce the severity and frequency of migraine attacks in some people, although, like every treatment, they don’t work for everyone.¹⁻³
The downside of occipital nerve blocks is that they have to be given by a health professional who knows how to do them, and they have to be repeated when the numbing effect of the anaesthetic on the nerves wears off. These factors can be barriers to accessing this treatment in Aotearoa New Zealand. You have to find a health professional willing and able to carry out the treatment, you have to be able to afford to pay them for it repeatedly and you have to be able to get an appointment with them when you need the next dose. Given the long wait times to see a GP, let alone a specialist, this can be the killer.
Botox
The other injection, which is only used to treat chronic migraine (when headache occurs for 15 days or more a month for at least three months), is onabotulinumtoxinA, more popularly known by its trade name of Botox. Botox contains a muscle relaxant from the bacteria Clostridium botulinum and is famous for erasing unwanted facial wrinkles. Its inclusion in the arsenal against chronic migraine was serendipitous. People with migraine who were having Botox injections for cosmetic reasons noticed they were also having fewer migraine attacks. Clinical trials to test out its effectiveness were done and a regime of 31–39 injections in the forehead, temples and neck were approved to treat chronic migraine, as the trials showed it did in fact reduce the pain and frequency of migraine attacks in a proportion of people.⁴
However, the same downsides of occipital nerve blocks apply to Botox. The injection regime has to be repeated every three months and if you can’t get it funded through the public health system, then it costs around $1,200 per session. Technically, Botox is funded for use in the hospital setting, such as neurology outpatient departments, but practically, it’s difficult for most people to access. Hospitals may choose not to pay for Botox from their medication budget or there may not be anybody at the hospital with the capacity, ability or interest in administering it to people with chronic migraine.
MiANZ 2022 survey results
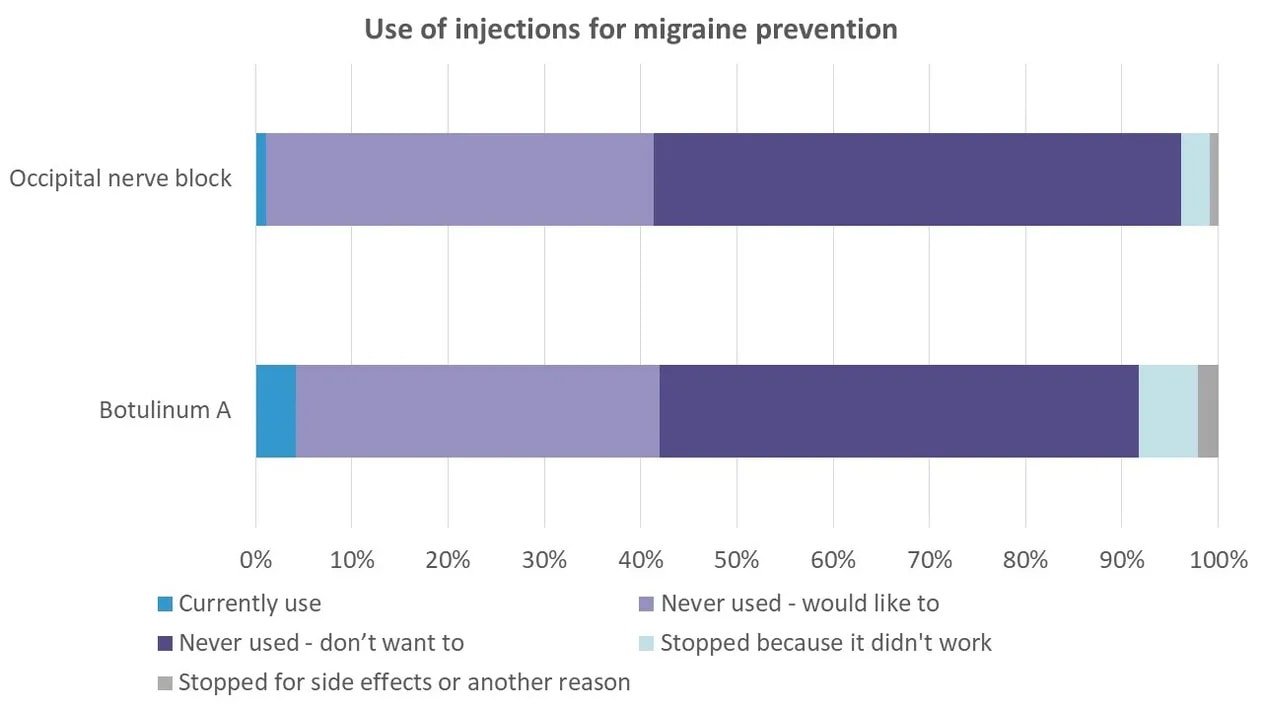
Given all of these issues, it was not surprising to find that very few people from the 2022 Migraine in Aotearoa New Zealand survey were currently using these injections. Less than 1% of respondents were using occipital nerve injections and barely 4% were using Botox. Another 4% had previously used occipital nerve injections and 8% had previously used Botox but had stopped, predominantly because they didn’t work. However, around 40% had never tried these but would like to.
Here’s another example of potentially effective and useful migraine treatments that are not available or being offered to people with migraine in New Zealand. We have a long way to go before we can say that everyone here has fair and equitable access to the full range of evidence-based treatments for migraine that are standard care elsewhere in the world.
References
- Velásquez-Rimachi, V. et al. Greater occipital nerve block for chronic migraine patients: A meta-analysis. Acta Neurol Scand 146, 101–114 (2022).
- Zhang, H., Yang, X., Lin, Y., Chen, L. & Ye, H. The efficacy of greater occipital nerve block for the treatment of migraine: A systematic review and meta-analysis. Clin Neurol Neurosurg 165, 129–133 (2018).
- Chowdhury, D. et al. Greater occipital nerve blockade for the preventive treatment of chronic migraine: A randomized double-blind placebo-controlled study. Cephalagia 43, 1–11 (2023).
- Kepczynska, K. & Domitrz, I. Botulinum Toxin-A Current Place in the Treatment of Chronic Migraine and Other Primary Headaches. Toxins (Basel) 14, (2022).


